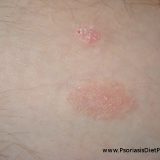
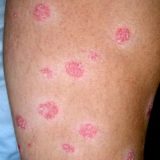
Ringworm Causes Psoriasis and It Is Contagious
Eventually psoriasis is really the fungus! Yes, it is the fungal infection of the skin and it is contagious. I am not saying that it is just fungal infection – Autonomic Nervous System dysfunction plays major role but what causes the primary immune reaction or suspected vasoconstriction in the skin? Scaly plaques are full of bacteria no doubt about that but the primary cause of immune reaction and the reason why psoriasis plaque develop may be the same as in…