Magnesium Is Not Depleted by Vitamin D3
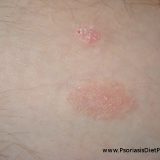
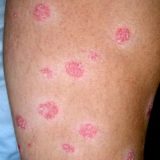
Psoriasis in many cases can be dramatically improved by vitamin D3 supplements. Even though there are opponents claiming D3 supplementation depletes magnesium stores vitamin D3 definitely helped a lot of psoriatics! Overview vitamin D significantly increases the magnesium absorption even though less than calcium absorption vitamin D does not cause magnesium loss vitamin D increases the bone resorption (rebuilding of the bone) magnesium significantly reduces the damage to arteries caused by hypervitaminosis D vitamin D activation needs magnesium, but this…