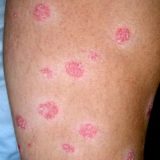
How Nystatin Cures Psoriasis
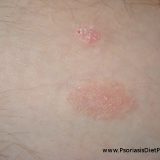
In this post I would like to support the connection between psoriasis, yeast infections and the fact that it is possible to cure psoriasis with Nystatin or some other antifungal drug. Nystatin is not the only option for intestinal yeast infection, but the advantage of Nystatin is that it is powerful fungistatic and fungicidal drug with low intestinal absorption. The fungistatic means that it does not kill the existing yeast cells but interferes with the growth of the new ones,…