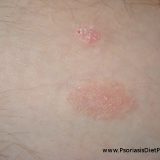
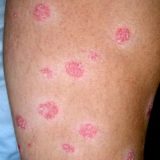
Is Anxiety Like OCD and Psoriasis Related?
Psoriasis as well as OCD which is a form of anxiety are both caused by excessive chronic inflammation. Sure! Those health problems are related! Even though OCD is considered to be a only a low serotonin issue and psoriasis the dysfunction of immune system both of those theories are wrong as they can be. Low Tryptophan Diet May Work for Psoriasis The idea of low tryptophan diet as psoriasis cure exists for about 48 years. All that begun in 1967…