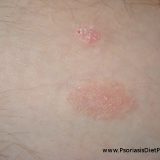
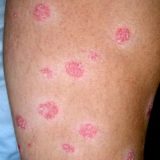
Psoriasis Is A Hypersensitive Response
You probably never heard this term in relation to psoriasis or any other chronic disease. Why? I don’t know because in other words I have been mentioning psoriasis being a hypersensitive protective mechanism for years on this blog. The science acknowledges the “hypersensitive response” exists in plants but why in the heck they don’t consider that there might be a chance that immune system in human body works the same way? Sorry, I did not tell you what a hypersensitive…