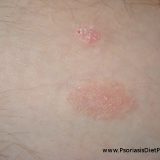
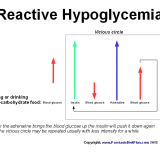
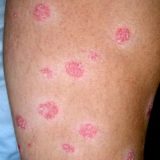
Sinusitis, Pituitary Tumor and Psoriasis Caused By Fungal Infection
Whether you have psoriasis, sinusitis, pituitary tumor or unfortunately all of those this blog post may come very handy to you. This will be about the ignorance, low professional intelligence and poor researching and professional qualities of many doctors out there. Psoriasis is a chronic inflammatory disease which is impossible to cure according to very most doctors in the world. Yes, we all know that and this blog is about all but the different view on this complex disease. But…