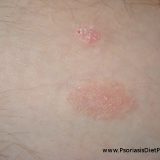
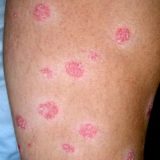
Alcohol Is Not As Bad For Psoriasis As You Think
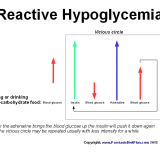
Alcohol is considered to be a risk factor for psoriasis but most people do not know why and how it may induce or worsen psoriasis. Now let me explain that… Alcohol directly does not cause psoriasis but at the same time it may significantly worsen it. Endotoxemia is perhaps the worst acute problem caused by alcohol consumption. The biggest part in psoriasis development in most people is probably the liver function. Liver is a major “biochemical factory” so when you…